Enterprise-wide care management (ECM) is a patient-centered approach to healthcare that eliminates the care siloes that may have evolved within healthcare organizations over time. ECM involves aligning care teams across a range of facility types, including acute care, skilled nursing facilities (SNFs), rehabilitation, ambulatory, home health, specialty, and community programs. The goal of ECM is that multiple complementary functions collaborate in one shared care plan across the enterprise so that communications and support surrounding a patient are effectively synchronized. This collaboration includes inpatient case coordination, transitions of care, disease coordination, complex care support, social determinants of health (SDoH) programs, behavioral health, and other functions.
How does ECM contribute to patient-centered care?
Enterprise-wide care management can benefit patients, healthcare providers, and the healthcare organization in many ways and make a meaningful impact on patient-centered care. Key value propositions include:
- Improved quality of care
- ECM allows for a more holistic view of a patient’s health. This facilitates informed decision-making by providers and promotes a more patient-centered approach to care. This can lead to better clinical outcomes and reduced readmission rates.
- Enhanced patient satisfaction
- Patients benefit from a streamlined and less fragmented care experience. Leveraging a strategic approach and healthcare technology, ECM promotes timely appointments, improved communication with providers, and better coordination between care settings, resulting in higher patient satisfaction.
- Increased efficiency
- ECM streamlines workflows, eliminates redundancies, and optimizes resource allocation within the organization. This leads to cost savings and allows healthcare providers to focus on delivering high-quality care.
- Improved population health management (PHM)
- In simple terms, PHM is a dedicated effort to improve the health outcomes of defined patient groups. ECM can help prevent chronic disease complications and reduce healthcare costs by identifying high-risk patient groups and proactively managing their care needs.
Patient-centered use cases for ECM in practice

Through an ECM model, streamlined communication with less care team members can efficiently collaborate and synchronize the patient’s care across relevant teams and resources. Receiving consistent information at appropriate intervals of time ensures optimum care and support specific to the patient’s needs.

Unified care teams in ECM models can address SDOH needs alongside clinical diagnoses. Coordination of care across relevant providers and community resources can include a wide range of roles, such an oncology social worker, community health navigator, virtual behavioral health support staff, inpatient case manager, pharmacy, oncologist, and others. This results in a personalized discharge plan, medication assistance, housing application assistance, transportation services, coordination of doctor appointments, and connection to a smoking cessation coach and behavioral health expert.
How is a unified care team structured under enterprise-wide care management?
Health systems have evolved with new care delivery models that may require additional teams to serve specific programming. If available, these additional care team members may focus on specific population needs or cohorts of patients. While beneficial to population health in theory, this approach can reduce progress because those teams may wear “care blinders” by focusing on only one aspect of care; they are not exposed to the entire care continuum for their patients. Moving away from this approach by establishing ECM is a cultural shift that requires an accountability structure that brings care teams together and reinforces collaboration and transparency.
An ECM leadership role must be established with oversight of clinical operations, managed care, community outreach, special SDOH programs, traditional home care, payer partnerships, physician affiliates, and innovative partnerships. This structure provides cross-continuum care management authority and commits the teams to a shared vision and plan. As the structure is established, new care team roles and responsibilities must also be outlined. During this process, leaders will gain a better understanding of skills that exist across the enterprise and where there are gaps. This visibility enables creative resource sharing across the enterprise to support all programs as the team gains cohesion and efficiency.
As the enterprise-wide team evolves with new roles and responsibilities, it is imperative to leverage defined KPIs to measure and monitor the value and return on investment of enterprise-wide care team collaboration. This enables leaders to communicate and celebrate the positive impact of ECM programs while identifying areas of opportunity.
Examples of meaningful metrics for ECM include:
- Care management episodes closed with a positive outcome
- Average time to triage referral
- Number of patients by case manager?
- Rate of SDOH screening?
- Percentage of care plan tasks/targets overdue
- Rates of chronic care management billing
- Patients with all HCC diagnoses refreshed
- Rates of transitional care management billing
- Episodes closed by outcome
- Patients with outstanding referrals
- Patients connected with community resources
- Average care plan task completion turnaround time
- Percentage of care plan tasks overdue
Best practices for implementing patient-centered care through enterprise care management include unified workflows for the care team. Structured support processes lead to better outcomes.
How can new workflows support the unified care team?
As the ECM care teams embrace new roles and responsibilities, it is critical to unify their workflows. Standardizing workflow processes with care protocols across the organization ensures consistent, high-quality care delivery. These protocols should address patient assessments, care pathway development, and referral processes.
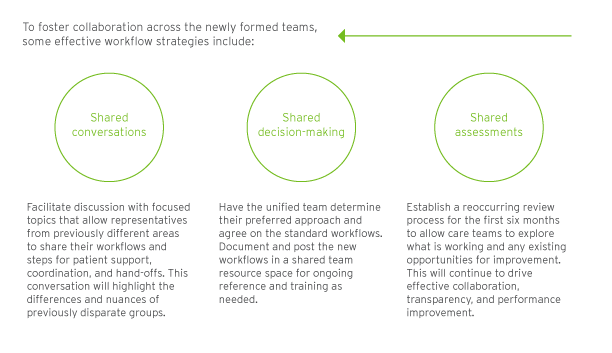
How does healthcare technology advance the success of ECM?
Like many investments in digital transformation, a digital health platform is a crucial enabler for organizations to drive enterprise-wide care management. The technology must be configured to provide a cohesive patient-centered care plan across the enterprise. This includes accessibility for all care team members to facilitate digital workflow collaboration, care plan management tools, real-time communication channels, and reporting and analytics capabilities.
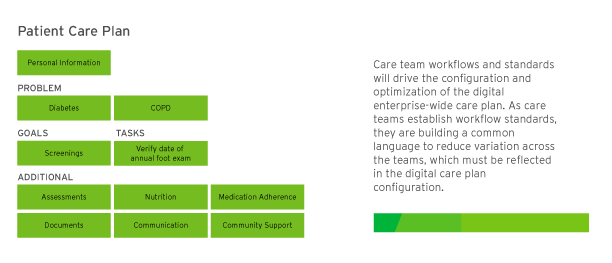

As technology is deployed across the healthcare organization, access to technologies is typically configured based on the location of a care team role. For example, an inpatient case manager role may only have access to see and document inpatient case manager-specific details. This means inpatient case managers cannot see any ambulatory information or other documentation input by disparate care team members for the same patient. As the new care team structure is established with new roles and responsibilities, configurations must be updated to enable the care team visibility to all program data, regardless of the care site.
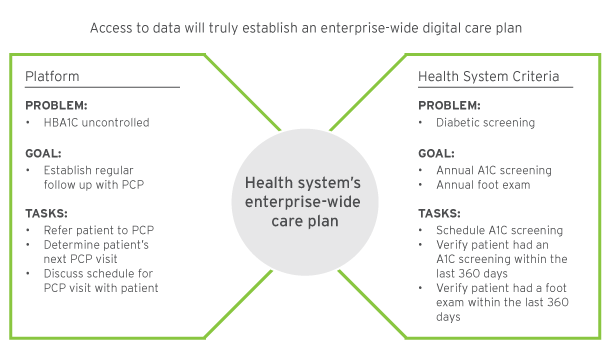
It is common for EHRs to offer foundational care plan capabilities. However, they will rarely meet the full needs of the care teams without customization. As care teams establish standard program workflows, they must document and share additional criteria needed with IT. For example, a foundational care plan to support diabetes may capture and help monitor HBA1C test results but not full diabetic screenings. A strong practice is to leverage program workflow decisions to drive digital care plan optimization.
How does ECM strategically align with population health and value-based care programs?
ECM can be fundamental to driving successful PHM, value-based care (VBC), and other care models. VBC is a healthcare delivery model designed to focus on quality of care, provider performance, and patient experience. The critical components of ECM that can contribute to the success of PHM and VBC initiatives success include:
- Organizational structure and governance that aligns roles, responsibilities, and accountability.
- Panel management access where actionable data and advanced accessibility help to manage patient portfolios through pre-visit, in-visit, and post-visit updates.
- Proactive care management aligns efforts to prevent care disruptions or adverse events and predict, identify, and prioritize care needs across the care continuum. Care gap management proactively identifies potential gaps and engages the patient to ensure they are closed for the best effect.
- Practice variation and total cost of care can embed evidence-based practice and streamlined workflows to match high-quality care efficiently.
- Payer contracting vision and strategy evaluates and optimizes payer contracting decisions.
- Provider and patient engagement ensures high satisfaction through customized technologies and personalized care experiences that address SDoH and health equity.
- Technology, data, and analytics capabilities coordinate and configure technology to provide deep insights for increased ease and efficiency.
- Risk adjustment captures accurate patient acuity for optimized reimbursement outcomes.
- Change management and benefits realization can be achieved by building a foundation encouraging adoption and sustainability.
When is the right time to move forward with ECM for a total transformation?
ECM represents a strategic shift towards a more integrated and coordinated approach to care delivery. As healthcare organizations work to modernize operating models, enterprise-wide care management is a fundamental element that will help propel the next phase of growth and financial sustainability. As the healthcare landscape continues to evolve, adopting an ECM approach is a pivotal step towards achieving sustainable success in our evolving healthcare landscape.
Learn how ECM transformation could apply to your organization through a 1:1 call with a Nordic expert.

