
As healthcare organizations continue to be squeezed by a myriad of factors, staff retention and recruitment are still of great concern. It is difficult to escape headlines around departmental closures due to staff shortages or long waitlists for access. In this environment, questions can arise as to the benefits or risks of implementing new technology. On the one hand, there is the belief that young, newly graduated practitioners are attracted to organizations with fully functional health information systems. On the other hand, you hear the cries of distress from clinicians going through implementations. So, we must ask: When it comes to recruiting and retaining staff, is technology an attractor or a deterrent? Spoiler: It depends on your approach to implementing it.
Let us first consider what factors lead to happiness, retention, and recruitment. From there, it is possible to examine the pros and cons of technology implementation according to those criteria. Fortunately, there are good data to help us.
A model for happiness, recruitment, and retention
Three areas of research align to form a model for the objective. The KLAS Arch Collaborative measures clinician satisfaction with their health information systems (HIS). With over 300,000 clinicians surveyed, the data show a strong correlation between quality education, personalization, and a healthy alliance between clinicians and IT. These criteria align with Susan Fowler’s well-researched components for improving motivation. Fowler finds that competency, autonomy (or choice), and connectedness (or relatedness) are the keys to motivated employees.1
Figure 1
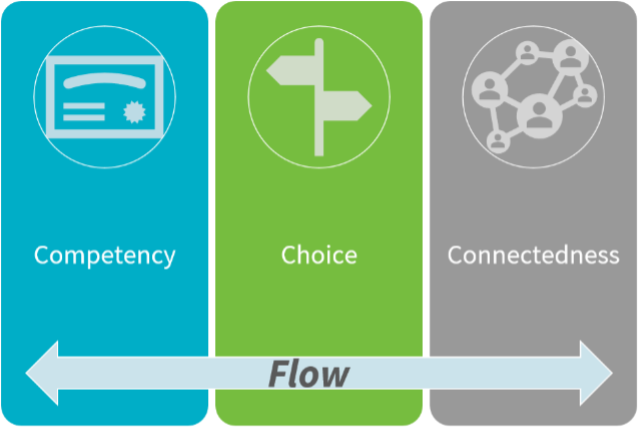 Underlying these common pillars of happiness is the foundation of a well-designed workflow. Mihaly Csikszentmihalyi, a pioneer in the study of happiness, defines flow as “a state in which people are so involved in an activity that nothing else seems to matter; the experience is so enjoyable that people will continue to do it even at great cost, for the sheer sake of doing it.”2
Underlying these common pillars of happiness is the foundation of a well-designed workflow. Mihaly Csikszentmihalyi, a pioneer in the study of happiness, defines flow as “a state in which people are so involved in an activity that nothing else seems to matter; the experience is so enjoyable that people will continue to do it even at great cost, for the sheer sake of doing it.”2
Establishing improved flow in healthcare practitioner’s (HCPs) work requires a critical eye on what improves the experience for both HCPs and patients alike. Currently, it is difficult to imagine achieving optimal flow in our healthcare setting. HCPs face numerous interruptions daily. Moreover, there is limited research in understanding the risks and benefits of interruptions in healthcare. An appropriately timed interruption can be the difference between administering a medication to which the patient is allergic and making a more personalized choice for that client. Alternatively, a meaningless alert can interrupt flow and cause a clinician to forget to complete a pathway or synthesize information.
Additional research into the factors that support HCP flow is sorely needed, but in the meantime, a healthy respect and curiosity can go a long way in approaching flow. With active clinician engagement, an eye to the pillars of satisfaction as outlined in the Arch Collaborative, and using the principles outlined by Fowler, an aspirational model can be created to guide us to improved work experiences and decreased burnout. Figure 1 represents a working model for establishing happiness, recruitment, and retention. With this data-informed model, we can see how it applies to technology implementation.
Starting afresh? Apply the Model.
HIS implementation is a wonderful opportunity to evaluate and redesign workflow. If this is done with a critical eye and the underlying goal of establishing flow for patients and HCPs, then significant improvements can be made beyond introducing new software. A beautiful workflow alone, however, will not solve the dissatisfaction inherent in implementations.
Figure 2
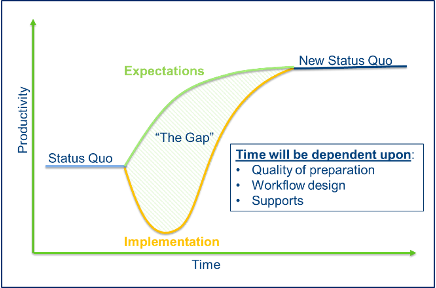
New implementations inevitably include grumblings best explained by the gap in the Jellison J-curve (Figure 2).3 People expect new systems to improve their workflow and efficiency. Otherwise, why would we implement them? What they overlook is the time it takes to rewire their brains to the new norm and the dip in productivity and happiness that is inevitable during that period. Applying the model to this situation, we can predict that proper education, an emphasis on customization for individual workflows, adequate support, and setting clear expectations can go a long way in establishing a tolerance for the temporary dip.
Is technology an attractor or a deterrent for recruiting and retaining staff? It will depend on the principles used to build it. An implementation done well, and with the criteria for happiness, recruitment, and retention in mind, can be an incredible asset to an organization.
Citations
- Fowler, S. (2014). Why motivating people doesn’t work… and what does. Berrett-Koehler.
- Csikszentmihalyi, M. (1990). Flow. The psychology of optimal experience. Harper Perennial.
- Jellison, J. (2006). Managing the dynamics of change: The fastest path to creating an engaged and productive workplace. McGraw Hill.
